
This is the second in a three-part blog series about COVID-19. Please also read Part 1 and Part 3.
I have been very moved by the responses my previous post has generated.
One can be easily numbed and unmoved by the steady drumbeat of bad news and misleading statistics produced by the news media. Sometimes personal stories can deliver more of an impact.
I had a lengthy chat with a friend who is an RN in an ICU in Portland. He provided a lot of information many outside health-care industry may not know.
Below are excerpts of my ICU RN friend’s comments interspersed with a few annotations of mine as well as comments from other friends and acquaintances who work in health care.
Update: I continue to receive messages from friends who provide medical care. I will update this post and its comments with their submissions.
I. The early phase of the COVID-19 Pandemic before vaccines were available.
Well, it’s definitely been a crazy 18 months through the pandemic. It has been strange how our perspectives as nurses have changed. There was so much uncertainty at the beginning … we were not sure what we were dealing with and how to manage it. But now it seems to have become almost routine in a sense … “yep another COVID patient.”
At the start [before vaccines were available] all of the patients were ones that just happened to catch the virus and were unlucky enough to be hospitalized in the ICU.
We felt so bad for these patients…. There were so many that the made a cut off on who could be intubated and put on a ventilator. You basically had to be 65 or less and have very few co-morbidities … then you would get a chance on the ventilator and hopefully your lungs would heal.
II. The ECMO Machine
Some were so sick that they were put on lung bypass or ECMO machine.
An ECMO machine (extracorporeal membrane oxygenation machine) is a heart-lung machine that can be used when a patient’s heart and/or lungs are too damaged to sufficiently supply the body with oxygen. It can be used in full heart-lung mode, or just lung mode.

These machines are rare. My friend estimates there may be two dozen ECMO machines in the Pacific Northwest and Alaska, and maybe 16 in the greater Portland area.
[ECMO machines were used for] the sickest of the sick when even a ventilator couldn’t help them. [An ECMO is] like heart by-pass in the OR, but this machine is for use at the bedside. We can set the machine up to just support the lungs. We were able to save a few but often the lungs were too damaged to even help with ecmo … it is a very very limited resource and takes 2 nurses at bedside.
III. Change of Heart
“My most recent patient was an older lady and did not get the vaccine because she was afraid of the side effects … she was now dying of COVID and wasn’t a candidate for a breathing tube.
IV. Frustration with the unvaccinated
I think a lot of us nurses are just exasperated at people who can get the vaccine and choose not to get it and then end-up in the ICU seriously ill … we have been dealing with COVID daily for the last 18 months …
I think like most things people don’t care until it personally impacts them in a negative way, sometimes even that doesn’t help …
Nursing is so much about care and compassion and you really have to dig deep when caring for patients that refuse to get vaccinated.
… for me in the ICU it is harder to get a whole lot of personal reflection with these type of patients because they are literally crashing when they arrive.
… a lot of the time we are just holding our tongue … as we prep them for intubation…. you just want to say “See, don’t you wish got your vaccine? You get this breathing tube instead .…”
Another RN friend wrote about being confounded by those who resisted the vaccines, but unquestioningly and readily accept hospitalization and drugs when they get very sick:
The comments [in your blog post] from people echo a lot of what I have seen in the last month. There have been some who, on their deathbed, say “I wish I would have gotten the vaccine” and conversely those who are adamant that even though they were on massive amounts of support and oxygen, leave the hospital and have no regrets about not opting for the vaccine. The curious thing is that a number of those with vaccine hesitancy related to concerns of what is in the vaccine and who end up in the hospital ask no questions — zero — regarding the medications we use to treat them.. namely remdesivir, dexamethasone, nebulizer breathing treatments, etc.
A college classmate who is an MD and professor of medicine at an Ivy League university wrote me:
I often wish it were a requirement for those who oppose vaccination (or masking) to spend one hour in an ICU watching a healthy 16 year old boy struggle to breathe and lose his battle. Or a woman in her third trimester never able to meet her child, and die alone as no visitors are allowed. Only then would I consider theirs a truly informed decision.
She wrote much more which I’ve copied in its entirety in the comments below.
V. Burnout
I’ve seen many news stories about nursing staff frustrated and exhausted with the long hours and exploding numbers of patients struggling and dying from COVID-19. Many are struggling with PTSD, and many are leaving the profession.

Nationwide, hospitals are offering hefty signing bonuses as well as large bonuses for overtime and extra shifts. From Portland to Philadelphia to Texas, hospitals are pulling out the stops to try to lure nurses to meet the burgeoning nursing demands due to COVID surges and nursing burnout.
I have heard anecdotally that these financial enticements are not enough to get shifts and positions filled. Many are simply unwilling to take on more hours and shifts after 18 months of facing this morbid Sisyphean task.
One of my RN friends is taking a break from the work. She’s been traveling and getting out in nature. She writes:
I really can’t handle thinking about it all the time, so when I’m in the woods, I try to give myself a true break – privileged as that is. The hospital is just too much.
Back to my ICU RN friend:
Yah it’s been crazy … work is so short-staffed and everyone is burned out. The ED gets the brunt of it but the ICUs are full too. There was 1 week in June that the ICU didn’t have a COVID a new COVID patient and we were all floored.
VI. The Dangers Health Providers Face
One friend whose daughter is an RN wrote me the following:
My RN daughter was fully vaccinated. She got COVID and was hospitalized 3 times. One time with a serious GI bleed which could have met death. It is a dangerous virus. There is one report of one man who was fully vaccinated who died of COVID but prior to him – zero.
As I wrote previously, full vaccination does not confer immunity, but for most people it can be enough protection to prevent the need for hospitalization. However, those in the front lines providing medical care are potentially much more heavily exposed to those who are infected with COVID-19.
VII. Grim Statistics
In the ICU death is a part of work – so in a sense experiencing dealing with it is part of the job.
Before the pandemic, the number of patients who died during his shifts was 2-4 in a year.
[In the past 18 months] I think personally maybe 30 or less [patients he treated died]
… I’d say of the patients I have cared for and passed, probably 99% [were COVID-related], there were a few traumas and heart attacks in there but I can say a majority have been COVID-related.
… Sometimes we’ll say, “Wow it’s been a while since a patient passed on me.” We don’t say that anymore….
VIII. The Rare Rewards
Despite the grim and challenging ongoing situation, my ICU RN friend is still keeping his chin up.
I actually do really well leaving work. I know I have a great team taking over my assignments and I have a superb ability to leave work at work. …. having great co-workers lends me that luxury.
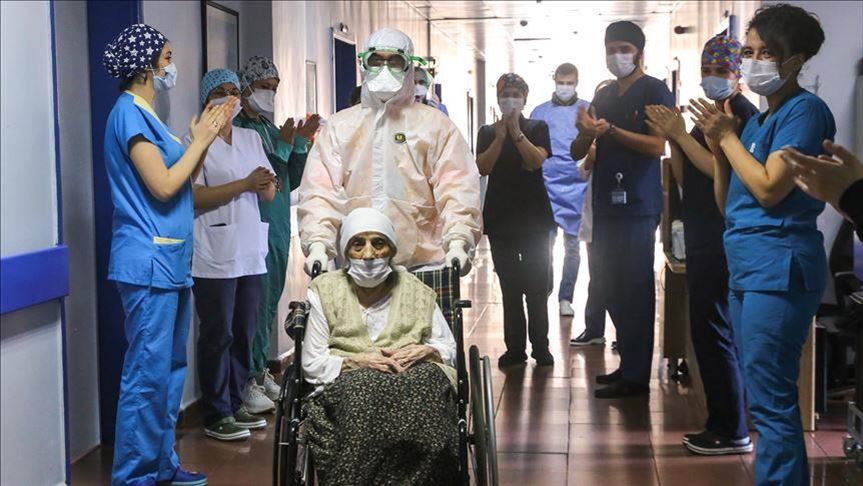
Definitely seeing a patient recover and get better makes everything worth it.
Conclusion
Even though I feel fairly knowledgeable about the pandemic and the dire situation facing our hospitals and caregivers, hearing firsthand accounts from personal friends providing care to patients carried a visceral punch from which I am still a bit stunned.
If you haven’t already, please read my prior post with stories about people who were hesitant or resisted the vaccine, then had a change of heart – sometimes too late.
Please wear your mask, practice physical distancing, wash your hands frequently, and most of all, get vaccinated and encourage everyone you know to do so!
The full text of the message I received from my college friend who is an MD and professor of medicine at an Ivy League University:
“It seems intuitive to receive a vaccine that not only confers protection against severe disease and mortality for oneself, but also for those around you, chief among them those too young to get vaccinated and those who are immunocompromised or have severe co-morbidities who would not fare well if they contracted the disease.
It also seems intuitive to wear a mask when indoors, given the substantial decrease in transmission if both infected individual and potential recipient are (1) both wearing masks and (2) maintaining physical distance. Vaccination of both individuals further decreases the chance of infectivity. Having to again wear masks is frustrating, it is restrictive and it is challenging. But it prevents infection (and thus morbidity and death). If your surgeon refused to wear a mask during your operation, would you defend her right to exercise her individual freedom?
I often wish it were a requirement for those who oppose vaccination (or masking) to spend one hour in an ICU watching a healthy 16 year old boy struggle to breath and lose his battle. Or a woman in her third trimester never able to meet her child, and die alone as no visitors are allowed. Only then would I consider theirs a truly informed decision.
When our medical system is overwhelmed as it currently is in much of the Southern US, people with pretty common problems like a heart attack or stroke – problems that in the current era given advances in care are not difficult to treat – will be and are being turned away because there are no beds. Doctors are unable to perform any but the most limited of surgical procedures without ventilators, and they are currently in short supply in many areas. Preventative health care is being deferred and many diagnoses are being delayed that would have been treatable had they been caught earlier.
Very sad state of affairs.”
LikeLike
Pingback: The virus does not care what you believe | Blatant Calm
Pingback: Pandemic 3: Showing Our Medical Staff Gratitude in the time of COVID-19 | Blatant Calm